Table of Contents
ToggleIntroduction: A Growing Environmental Concern
The connection between microplastics and Parkinson’s disease has become one of the most closely watched areas of emerging neuroscience. Scientists are now asking a question that would have seemed far-fetched just a decade ago: could the same microscopic plastic particles polluting our oceans, food supply, and drinking water also be quietly disrupting the human brain? Early evidence suggests the answer may be yes — and patients, caregivers, and clinicians have good reason to pay attention.
Parkinson’s disease affects more than 10 million people worldwide and over 1 million Americans, making it the second most common neurodegenerative disorder after Alzheimer’s disease. Its hallmark features — tremor, rigidity, slowness of movement, and postural instability — result from the progressive loss of dopamine-producing neurons in the brain. While genetics explains fewer than 10% of cases, environmental triggers are widely suspected to play a major role in the remaining majority. Accordingly, the rapid accumulation of microplastics and nanoplastics in the human body over recent decades has become a subject of urgent scientific scrutiny.
This article reviews the current state of research on microplastics and Parkinson’s disease, explores the biological mechanisms that make this connection plausible, and outlines how Ayurvedic medicine — the ancient healing system of India — approaches Parkinson’s through detoxification, neuroprotection, and holistic restoration. The goal is to give readers both an honest picture of what science currently knows and a broader framework for comprehensive care.
Part One: The Science of Microplastics and Parkinson’s Disease
What Are Microplastics and Where Are They Found?
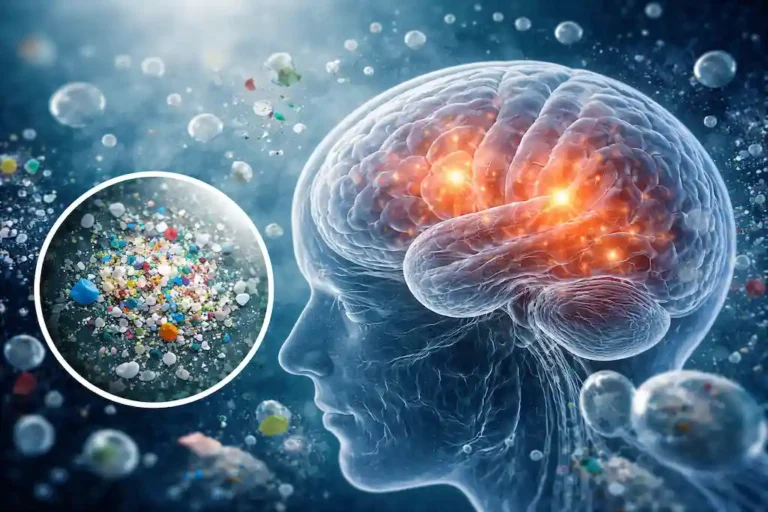
Microplastics are plastic fragments smaller than five millimeters in diameter. They originate from the breakdown of larger plastic products, industrial processes, synthetic textiles, and personal care products containing microbeads. Nanoplastics — a subset of this category — are even smaller, often invisible to the naked eye, and more biologically active due to their ability to penetrate cell membranes and cross physiological barriers.
These particles are now found virtually everywhere: in drinking water, sea salt, shellfish, bottled beverages, the air we breathe, and even in human blood, placental tissue, and lung samples. In short, microplastic exposure is no longer a future risk — it is an ongoing, daily reality for virtually every person on Earth. Because these particles enter the body through ingestion, inhalation, and possibly skin absorption, researchers are increasingly focused on understanding their long-term effects on human health, including neurological function.
How Microplastics May Affect the Brain
Research into the relationship between microplastics and Parkinson’s has accelerated considerably in recent years. Several biological mechanisms have been identified through laboratory and animal studies that help explain why plastic particle exposure could be particularly dangerous for the nervous system.
Oxidative Stress and Neuroinflammation. Scientific reviews have demonstrated that microplastics and nanoplastics trigger oxidative stress and cellular inflammation in animal and laboratory models. Oxidative stress occurs when harmful free radicals overwhelm the body’s natural antioxidant defenses, damaging cells in the process. Neuroinflammation — chronic inflammation within the brain — is already well-established as a central driver of Parkinson’s pathology. When researchers expose neural cells to plastic particles, they observe activation of inflammatory pathways that closely mirror those seen in Parkinson’s patients (Prüst et al., 2020; Yong et al., 2020).
Mitochondrial Dysfunction. Mitochondria are the energy-producing organelles inside every cell, and their failure is a defining feature of Parkinson’s disease. Toxicology studies consistently show that nanoplastics can disrupt mitochondrial function and reduce cellular energy production. Because dopaminergic neurons are especially energy-dependent, this type of mitochondrial stress makes them particularly vulnerable to plastic-induced damage (Yong et al., 2020).
Protein Misfolding and Alpha-Synuclein Aggregation. One of the most significant discoveries in Parkinson’s research is the role of a protein called alpha-synuclein. In healthy brains, this protein circulates normally. However, in Parkinson’s disease, alpha-synuclein misfolds and clumps together into toxic aggregates known as Lewy bodies. These deposits progressively destroy dopamine-producing neurons. Emerging laboratory evidence suggests that exposure to certain environmental particles may accelerate protein misfolding and neuronal stress — and that nanoplastics may actively promote the formation of these pathological alpha-synuclein aggregates (Prüst et al., 2020). This is a particularly alarming finding, given that once Lewy body propagation begins, it can spread from neuron to neuron in a manner that resembles a prion-like cascade.
Crossing the Blood-Brain Barrier. Perhaps the most alarming characteristic of nanoplastics is their capacity to cross the blood-brain barrier — the highly selective filtration system that protects the brain from most foreign substances. A 2026 review published in npj Parkinson’s Disease examined emerging evidence on environmental contaminants — including micro- and nanoplastics — that may influence Parkinson’s pathology precisely through this mechanism (Lin et al., 2026). Once inside brain tissue, plastic particles may interfere with cellular waste-removal systems and disrupt protein regulation, two processes that are already compromised in Parkinson’s disease.
Animal Research: Worsened Neurological Outcomes
Beyond cell culture experiments, animal studies have shown that nanoplastic exposure leads to measurably worse neurological outcomes. Rodents exposed to plastic particles demonstrate increased neuroinflammation, greater dopaminergic neuron loss, and impaired motor function compared to controls. While animal models do not perfectly replicate human disease, these findings reinforce the biological plausibility of a microplastics–Parkinson’s connection and justify urgent further investigation.
The Gut-Brain Connection: A Key Puzzle Piece
One of the most intriguing threads in Parkinson’s research concerns the gut. Scientists now know that in many patients, the misfolding of alpha-synuclein appears to begin not in the brain, but in the gastrointestinal tract — specifically in the autonomic nerve networks of the colon and rectum. This misfolded protein then appears to travel via the vagus nerve upward into the brainstem, before eventually reaching the substantia nigra where it destroys dopamine-producing cells. Since microplastics are ingested primarily through food and water and accumulate in the gastrointestinal tract, this gut-origin theory of Parkinson’s disease adds another reason to investigate the specific role of microplastics and Parkinson’s development.
What the Evidence Does — and Does Not — Show
It is important to be clear about what current science establishes. The body of evidence linking microplastics and Parkinson’s currently demonstrates mechanistic plausibility — meaning that plastic particles can trigger the exact biological processes that drive Parkinson’s disease progression. However, confirmed causation in humans has not yet been established, largely because long-term human cohort studies on this specific question are still in early stages.
Clinical Note: Researchers caution that current evidence shows mechanistic plausibility, not confirmed causation. Most studies involve laboratory and animal models rather than long-term human trials. Nevertheless, the widespread presence of microplastics in modern environments has prompted urgent calls for further investigation.
Despite this limitation, the 2026 review by Lin and colleagues represents an important step forward, synthesizing available evidence and identifying priority directions for future research. As plastic production shows no signs of slowing, and human microplastic body burdens continue to rise, the urgency of understanding this relationship grows alongside it.
Part Two: Ayurvedic Understanding of Parkinson’s Disease (Kampavata)
Ancient Recognition of a Modern Disease
While Western medicine formally identified Parkinson’s disease only in the 19th century, Ayurveda — the classical medical system of India — recognized and described an equivalent condition thousands of years earlier. In Ayurvedic texts, Parkinson’s disease corresponds to a disorder called Kampavata (from the Sanskrit kampa, meaning tremor, and vata, one of the three fundamental biological energies or doshas). References to whole-body tremor, head shaking, slowness of movement, postural changes, speech difficulties, and even cognitive decline appear in classical Ayurvedic literature dating back to the 7th century AD through the 18th century, mapping remarkably closely onto the modern clinical picture of Parkinson’s disease.
Dr. Scott Gerson, MD, Ph.D. (Ayurveda), writing through the Gerson Institute of Ayurvedic Medicine, has elaborated extensively on this parallel. Particularly noteworthy is the Ayurvedic observation that the disease originates in the colon — the primary seat of Vata dosha in Ayurvedic physiology — before spreading through subtle channels to the brain. This parallels the modern scientific discovery that Parkinson’s pathology frequently begins in the gastrointestinal tract and travels upward to the brain via the vagus nerve.
The Ayurvedic Pathophysiology of Kampavata
In Ayurvedic theory, Parkinson’s disease is primarily a disorder of Vata dosha — the biological energy associated with movement, communication, and nervous system function. When Vata becomes excessively aggravated through stress, aging, poor diet, inadequate sleep, and exposure to environmental toxins, it accumulates first in the colon. If unchecked, it then overflows into the circulatory system and ultimately relocates to Majja Dhatu — the nervous tissue — where it causes progressive dysfunction.
Kampavata also involves disruptions in Pitta dosha (manifesting as neuroinflammation) and Kapha dosha (manifesting as the accumulation of toxic protein aggregates — strikingly analogous to Lewy bodies of alpha-synuclein). This multi-dosha framework means that comprehensive Ayurvedic treatment must address all three layers of pathology simultaneously.
Part Three: Ayurvedic Treatment Strategies for Kampavata
Ayurvedic treatment of Kampavata is comprehensive and individualized. It proceeds in distinct phases: first purification, then rebuilding and nourishment. Because this is a complex condition involving both tissue depletion and channel blockage, treatment typically requires a sustained, multifaceted commitment.
Phase One: Panchakarma — Deep Purification
Panchakarma is the cornerstone of Ayurvedic management for Kampavata. These classical detoxification therapies are designed to remove accumulated toxins (ama), correct dosha imbalances, and restore the proper flow of energy through the body’s channels (srotamsi). Treatment proceeds in a deliberate sequence, with each therapy preparing the body for the next.
Snehana (Internal and External Oleation): The first step involves oleation therapy in both internal and external forms. Patients typically ingest pure cow’s ghee for four to seven days to lubricate tissues from within and mobilize deeply seated ama. Simultaneously or subsequently, Abhyanga — a warm herbal oil massage using formulations such as Dashamoola bala taila, sahacharadi taila, or narayana taila — is administered to calm the nervous system, improve muscular flexibility, and direct loosened toxins toward elimination pathways. Specific marma points (energetic junctions on the body) are addressed throughout as indicated by the patient’s presentation.
Swedana (Herbal Steam Therapy): Following oleation, Swedana — whole-body herbal steam treatment — dilates the body’s channels and promotes elimination through perspiration. In bashpa swedana, the body is enveloped in medicated steam while the head remains outside the chamber. This therapy relaxes rigid musculature, enhances peripheral circulation, and further prepares tissues for deeper cleansing. Because significant changes in blood pressure and pulse can occur during the procedure, careful monitoring is essential throughout.
Virechana (Therapeutic Purgation): This guided cleansing protocol uses gentle herbal purgatives — traditionally castor oil (eranda taila) — to systematically eliminate accumulated Vata and Pitta doshas from the gastrointestinal tract. Because the colon is the primary site of Vata accumulation in Kampavata, purifying it is therapeutically central rather than peripheral. Following purgation, patients observe a prescribed light dietary regimen (samsarjana krama) for four to seven days — progressing from rice water to simple kitchari — before resuming a normal diet.
Basti (Therapeutic Enema Therapy): Considered the single most important Panchakarma treatment for Kampavata, basti involves the alternating administration of oil-based (anuvasana) and herbal decoction-based (niruha) enemas directly into the colon over 8, 14, or 21-day courses. Because the colon is the primary seat of Vata dosha, basti delivers therapeutic substances precisely to the site where Kampavata originates — making it uniquely effective among all available interventions. Classical Ayurvedic texts are unambiguous on this point: Kampavata cannot be effectively treated without basti chikitsa. This traditional conviction now has meaningful clinical support. A 2025 comprehensive narrative review published in Cureus (Chikkanna et al., 2025), analyzing seven clinical trials of Ayurvedic interventions for Parkinson’s disease, found that the combination of Panchakarma bio-cleansing with Mucuna pruriens outperformed either therapy used in isolation — the only trial in the review to test this combined approach, and a finding that directly validates the integrated treatment model that Ayurveda has advocated for centuries.
Nasya (Medicated Nasal Therapy): Nasya involves the administration of medicated oils through the nasal passages to directly nourish the brain and nervous system. This therapy is particularly relevant in Kampavata given the frequency of anosmia (loss of smell), cognitive changes, and speech difficulties that accompany the condition. Because the nasal passages provide a relatively direct route to the central nervous system, nasya is considered a primary delivery pathway for neuroprotective herbal compounds — and is among the first therapies initiated when symptoms involve the head and upper neurological regions.
Phase Two: Herbal Medicines and Rasayanas
Following purification, Ayurvedic care transitions to rebuilding and nourishing the nervous system through carefully selected herbal medicines. These fall into two categories: aushadhis (specific medicines targeting the disease) and rasayanas (broader tonics that promote vitality, longevity, and tissue regeneration). In Kampavata, both are typically administered concurrently.
Mucuna pruriens (Kapikacchu): Perhaps the most scientifically validated herb in the Kampavata pharmacopoeia, Mucuna pruriens contains naturally occurring L-DOPA — the same dopamine precursor used in conventional Parkinson’s medications. Importantly, this is no longer just traditional claim. A 2025 comprehensive narrative review published in Cureus (Chikkanna et al., 2025), analyzing seven clinical trials of Ayurvedic interventions for Parkinson’s disease, found that Mucuna pruriens consistently extended the patient’s “ON state” — the therapeutic window during which medication is working effectively — and measurably improved motor symptoms even in individuals with advanced PD. Notably, it did so with a more favorable side effect profile than standard levodopa/carbidopa. One trial included in the review demonstrated that combining Mucuna with Panchakarma bio-cleansing outperformed either intervention used alone, underscoring the value of the integrated Ayurvedic approach (Chikkanna et al., 2025). A separate review in the Journal of Ethnopharmacology also identified Mucuna as a strong candidate for adjuvant therapy alongside conventional drugs rather than as a replacement (Pathak-Gandhi & Vaidya, 2017).
Dashamoola (Ten Roots Formula): Dashamoola is one of the most consistently used formulations across published clinical case studies of Kampavata management, appearing in multiple forms. As Dashamoola bala taila — a medicated oil — it is applied during Abhyanga massage and Patrapinda Swedana (bolus massage) for its potent Vatahara (Vata-pacifying) properties. As a kwatha (herbal decoction), it serves as the medium for Svedana steam therapy. Additionally, Dasamoolarishta — a traditional fermented medicinal preparation containing Dashamoola alongside Ashwagandha, Bala, and other herbs — is administered orally as both a Vata-balancing medicine and a restorative tonic (Suraksha et al., 2023; Mandal et al., 2019).
Ashwagandha (Withania somnifera): Long valued in Ayurvedic tradition as a premier nervine tonic and adaptogen, Ashwagandha has also been the subject of translational pharmacological research. Pathak-Gandhi and Vaidya (2017) specifically identified Withania somnifera as demonstrating documented neuroprotective effects on dopaminergic neurons in contemporary research — giving this classical herb meaningful scientific grounding beyond its traditional reputation. It is commonly administered as a churna (powder), arishta (medicinal wine), or ghrita (herbalized ghee).
Brahmi (Centella asiatica / Bacopa monnieri): These classical nervine rasayanas nourish Majja Dhatu (nervous tissue) directly, supporting memory, cognitive clarity, and neurological resilience. Brahmi ghrita is among the most esteemed formulations for delivering these compounds in a fat-soluble medium capable of crossing lipid membranes.
Amalaki (Emblica officinalis) and Guduchi (Tinospora cordifolia): Both are foundational antioxidant and immunomodulatory herbs used to counteract the oxidative stress and systemic inflammation that drive neurodegeneration. Their inclusion reflects Ayurveda’s recognition that Parkinson’s is not purely a motor disorder but a systemic inflammatory condition — a view now strongly supported by modern neuroscience.
Herbalized Ghees (Ghritas): Formulations such as Brahmi ghrita and Saraswata ghrita deliver fat-soluble neuroprotective compounds directly to the nervous system, taking advantage of ghee’s unique capacity to carry medicinal substances across lipid membranes — including, potentially, the blood-brain barrier.
Phase Three: Yoga, Pranayama, and Meditation
Lifestyle therapeutics are considered as essential as herbal medicines in Ayurvedic care for Kampavata. Specifically:
- Gentle Yoga Asanas: Slow, precise, and restorative yoga postures address the postural instability, rigidity, and balance difficulties characteristic of Parkinson’s. Postures such as Tadasana (Mountain Pose), Vrksasana (Tree Pose), and Virabhadrasana II (Warrior Pose II) have been found to improve range of motion, decrease rigidity, and — importantly — restore confidence and positive emotional experience in patients who feel increasingly uncertain in their bodies.
- Pranayama (Controlled Breathing): Pranayama techniques engage the diaphragm, oxygenate the lower lobes of the lungs, and deliver increased oxygen to the brain. Practices such as Nadi Shodhana (alternate nostril breathing), Bhramari (humming breath), and Kapalabhati are particularly recommended for Kampavata. They calm stress responses, regulate the autonomic nervous system, and support respiratory strength — which can decline as Parkinson’s progresses.
- Dhyana (Meditation): Regular meditation practice integrates the intellectual, emotional, and volitional dimensions of the mind. For Parkinson’s patients, who often experience depression, anxiety, and cognitive changes alongside their motor symptoms, this integrative dimension of treatment is especially significant.
Diet: A Vata-Reducing Approach
Dietary recommendations center on foods that pacify Vata dosha: warm, moist, nourishing, easily digestible meals with adequate healthy fats and sufficient fiber. Organic foods are strongly preferred. Cold, raw, dry, and highly processed foods are avoided as they aggravate Vata and worsen neurological instability. Consistent meal timing and a calm, unhurried eating environment are also emphasized as part of lifestyle management.
Part Four: Integrating Modern Research and Ayurvedic Care
The emerging science of microplastics and Parkinson’s disease and the ancient science of Kampavata are more complementary than they might initially appear. Both frameworks recognize that Parkinson’s disease is driven — at least in part — by environmental toxins that accumulate in the body, trigger inflammation, disrupt protein homeostasis, and progressively damage the nervous system. Modern toxicology identifies plastic particles as potential accelerants of this process; Ayurveda offers thousands of years of systematic methodology for removing precisely those kinds of accumulated toxins, reducing neuroinflammation, and restoring neurological resilience. Furthermore, the fact that microplastics and Parkinson’s research increasingly points to the gut as a critical site of disease initiation aligns strikingly with Ayurveda’s millennia-old insistence that Kampavata originates in the colon — a convergence that is difficult to dismiss as coincidence.
What is particularly encouraging is that Ayurvedic interventions for Parkinson’s are no longer supported only by classical texts and traditional practice. Peer-reviewed clinical research is beginning to validate what Ayurvedic physicians have prescribed for centuries. The 2025 Cureus review by Chikkanna and colleagues, drawing on seven clinical trials, demonstrated that Mucuna pruriens extended the therapeutic window for Parkinson’s patients and improved motor function even in advanced disease — with a safety profile that compared favorably to standard pharmaceutical options. Equally significant, the one trial that combined Panchakarma detoxification with Mucuna pruriens produced superior outcomes to either approach alone, offering clinical evidence for the integrated model that sits at the heart of Ayurvedic care. Translational research has also documented neuroprotective effects of Withania somnifera on dopaminergic neurons, lending further scientific grounding to the classical herbal pharmacopoeia (Pathak-Gandhi & Vaidya, 2017).
From a practical standpoint, this convergence means that patients and families navigating Parkinson’s disease today have access to a broader and better-supported set of tools than conventional neurology alone can provide. The Ayurvedic emphasis on individualized assessment, systematic purification, neuroprotective botanicals, and lifestyle integration does not replace conventional medications such as levodopa/carbidopa — but it may meaningfully complement them by addressing dimensions of the disease that pharmaceuticals cannot reach. Moreover, the microplastics and Parkinson’s research trajectory points toward the growing importance of environmental awareness and active prevention. Reducing plastic exposure where possible — filtering drinking water, minimizing food packaged in plastic, choosing glass or stainless steel containers, and prioritizing fresh organic whole foods — aligns naturally with the dietary and lifestyle principles that Ayurveda has long advocated.
Conclusion
The scientific conversation surrounding microplastics and Parkinson’s disease is still evolving. Nevertheless, the early findings are significant: plastic particles can trigger oxidative stress, neuroinflammation, mitochondrial dysfunction, and alpha-synuclein misfolding — every one of the core biological processes that drive Parkinson’s disease progression. Animal studies demonstrate measurably worse neurological outcomes following nanoplastic exposure, and a 2026 review in npj Parkinson’s Disease has synthesized the evidence and identified plastic particles capable of crossing the blood-brain barrier as a priority area of investigation (Lin et al., 2026).
At the same time, the Ayurvedic tradition’s ancient description of Kampavata — including its intuitive identification of the colon as the disease’s origin site — demonstrates that a holistic understanding of Parkinson’s pathophysiology is not new. Rather, it is a rediscovery. The Panchakarma purification system, neuroprotective herbal medicines, restorative yoga practices, and Vata-balancing dietary protocols collectively offer an integrative roadmap for supporting the Parkinson’s patient far beyond what symptom management alone can provide.
As research into microplastics and Parkinson’s continues to progress, understanding this relationship will remain essential for developing prevention strategies and next-generation therapeutic approaches. In the meantime, combining the best of modern neurological care with the deep wisdom of Ayurvedic medicine offers patients and their families a more complete, more hopeful path forward.
References
- Lin, L., et al. (2026). Micro-nanoplastics and Parkinson’s disease: evidence and perspectives. NPJ Parkinson’s Disease, 12(1), 56.
- Prüst, M., Meijer, J., & Westerink, R. H. S. (2020). The plastic brain: neurotoxicity of micro- and nanoplastics. Particle and Fibre Toxicology, 17, 24.
- Yong, C. Q. Y., Valiyaveettil, S., & Tang, B. L. (2020). Toxicity of Microplastics and Nanoplastics in Mammalian Systems. International Journal of Environmental Research and Public Health, 17(5), 1509.
Chikkanna, U., Venkatram, S., Holla, B., Mahale, R.R., Bhargav, H., Jasti, L.N., Ramakrishna, K.K., & Varambally, S. (2025). Exploring Ayurveda’s potential in Parkinson’s disease: A comprehensive narrative. Cureus, 17(10), e93992.
Pathak-Gandhi, N., & Vaidya, A.D.B. (2017). Management of Parkinson’s disease in Ayurveda: Medicinal plants and adjuvant measures. Journal of Ethnopharmacology, 197, 46–51.
Suraksha, S., et al. (2023). Ayurvedic management of Parkinson’s disease: A case study. Journal of Ayurveda and Integrated Medical Sciences, 8(1), 198.
Mandal, S., Sawarkar, P., Singh, V., Parwe, S., & Sawarkar, G. (2019). Managing Kampavata (Parkinson’s disease) through Ayurveda: A case study. Journal of Ayurveda Case Reports.
Microplastics and Parkinson's FAQs
What is the link between microplastics and Parkinson's disease?
A 2026 review in npj Parkinson's Disease identified micro- and nanoplastics as environmental contaminants capable of crossing the blood-brain barrier and disrupting the cellular processes central to Parkinson's pathology (Lin et al., 2026).
While confirmed causation in humans has not yet been established, the biological mechanisms identified are the same ones that drive Parkinson's progression.
Are microplastics found in the human brain?
Once inside brain tissue, they may interfere with cellular waste-removal systems and protein regulation.
The implications for neurodegenerative diseases like Parkinson's are an active and urgent area of scientific investigation.
What did the 2026 study on microplastics and Parkinson's disease find?
The review identified several mechanisms of concern: plastic particles crossing the blood-brain barrier, disrupting protein homeostasis, accelerating alpha-synuclein misfolding, and promoting neuroinflammatory signaling.
The authors identified this as a priority area for future human cohort research and called for further investigation into exposure reduction as a potential prevention strategy.
Can microplastics trigger the same brain changes seen in Parkinson's disease?
Additionally, nanoplastic exposure has been shown to promote the aggregation of alpha-synuclein into the toxic protein clumps that characterize Parkinson's pathology.
Animal studies have demonstrated measurably worse neurological outcomes, including greater dopaminergic neuron loss and impaired motor function, following nanoplastic exposure.
Is there a connection between microplastic exposure and gut health in Parkinson's disease?
Scientists have established that in many Parkinson's patients, the disease process appears to begin in the gastrointestinal tract, specifically in the autonomic nerve networks of the colon, before traveling via the vagus nerve to the brain.
Since microplastics enter the body primarily through ingestion and accumulate in the gut, this gut-origin theory of Parkinson's disease makes the microplastics connection particularly significant.
Interestingly, Ayurvedic medicine identified the colon as the origin point of Kampavata (its equivalent of Parkinson's disease) thousands of years before modern science confirmed the gut-brain pathway.
How can I detox microplastics from my body?
Ayurvedic Panchakarma therapies, including Abhyanga (herbal oil massage), Swedana (herbal steam), Virechana (therapeutic purgation), and Basti (therapeutic enema therapy targeting the colon directly), are specifically designed to mobilize and eliminate accumulated toxins from deep tissues.
Additionally, reducing ongoing exposure is critical: filtering drinking water, avoiding plastic food packaging, choosing fresh organic foods, and minimizing use of synthetic personal care products all meaningfully reduce your daily microplastic intake.
Supporting gut health through fiber-rich foods, fermented foods, and anti-inflammatory herbs further aids the body's elimination capacity.
What Ayurvedic treatments are used for Parkinson's disease?
The first phase involves Panchakarma detoxification, including Abhyanga oil massage, Swedana steam therapy, Virechana purgation, Basti enema therapy, and Nasya nasal oil therapy.
The second phase emphasizes rebuilding the nervous system through herbal medicines including Mucuna pruriens (which contains natural L-DOPA), Dashamoola (a ten-root formula used in oils, decoctions, and medicinal wines), Ashwagandha, Brahmi, Amalaki, and Guduchi.
The third phase incorporates gentle yoga, pranayama breathing practices, meditation, and a Vata-reducing diet.
All Ayurvedic treatment should be supervised by a qualified practitioner and used alongside, not instead of, conventional neurological care.
Is Mucuna pruriens effective for Parkinson's disease?
It contains naturally occurring L-DOPA, the same dopamine precursor used in standard Parkinson's medications.
A 2025 comprehensive review published in Cureus, analyzing seven clinical trials, found that Mucuna pruriens consistently extended the patient's therapeutic "ON state," improved motor symptoms even in advanced Parkinson's disease, and demonstrated a more favorable side effect profile compared to standard levodopa/carbidopa (Chikkanna et al., 2025).
One trial showed that combining Mucuna with Panchakarma detoxification produced superior outcomes to either treatment alone.
Can Ayurveda help with microplastic detoxification specifically?
Panchakarma therapies are designed to remove ama (metabolic and environmental toxins) from deep tissues, improve elimination through the colon, skin, and respiratory tract, and restore the integrity of the body's channels.
The colon-focused therapies (Virechana and Basti) are particularly relevant given that microplastics accumulate in the gastrointestinal tract and the gut is now understood as a key site of Parkinson's disease initiation.
Supporting detoxification through Ayurvedic principles, combined with reducing ongoing plastic exposure, represents a rational integrative strategy.
How can I reduce my risk of microplastic exposure to protect brain health?
Eating lower on the marine food chain (smaller fish accumulate fewer plastics), choosing natural fiber clothing and furnishings where possible, and ventilating indoor spaces regularly can also help.
These measures will not eliminate exposure entirely, microplastics are now pervasive in the environment, but they can substantially reduce your daily body burden.
What is the Ayurvedic view of environmental toxins and neurological disease?
The Ayurvedic framework holds that toxins accumulating in the gastrointestinal tract, if not cleared, eventually enter the circulation and relocate to vulnerable tissues including the nervous system.
This perspective predates modern environmental medicine by thousands of years, yet maps closely onto current scientific understanding of how environmental exposures, including microplastics and Parkinson's disease risk, may interact with genetic susceptibility to trigger neurodegeneration.
Should someone with Parkinson's disease try Ayurvedic treatment?
Clinical research is increasingly supportive: peer-reviewed trials have documented benefits of Mucuna pruriens and Panchakarma for motor symptoms, and translational research confirms neuroprotective properties of several classical Ayurvedic herbs.
However, Ayurvedic treatment should always be undertaken under the supervision of a qualified Ayurvedic physician and in coordination with the patient's neurologist.
It is not a replacement for conventional care, it is a powerful addition to it.